Katie Turner from The Institute of Voluntary Action Research recently published a case study based on interviews with stakeholders in the SAPA 5 Personalised Care Team (PCT) entitled ‘A new approach to personalised care in SAPA 5: Connecting Health Communities in Sheffield’.
It is based on the SAPA 5 neighbourhood of Sheffield and explores a partnership approach to developing a personalised healthcare system that brings together the combined experience of the health and voluntary sector.
The case study explores what working in this way has achieved, some of the challenges encountered along the way, and what is required to sustain and build on the work of this PCT. This case study hopes to support other places looking to develop their approach to personalised care.
SAPA 5 Primary Care Team
The PCT has been in formation for the last three years and came together from existing partnership working between SAPA 5 and the community anchor organisation SOAR that works with partner organisations and residents to provide a range of services designed to improve a person’s health wellbeing and employability through community development approaches.
SOAR provides one of the largest social prescribing services in the city and is working in partnership with three Primary Care Networks (PCNs) and Community Partners across the City. The operational management of the PCT is overseen by SOAR and the Clinical Specialist Occupational Therapist (with input from Sheffield Futures) and is supported by the PCN via the Clinical Director and Network Manager. The different roles that make up the PCT are either employed by SOAR, Sheffield Futures, the PCN or seconded from Sheffield Health and Social Care (SHSC).
The SAPA 5 PCT referrals come from GP services in the locality for people with complex health needs that cannot be met by existing services. Using the PCT’s combined knowledge and skills, they can work together to identify what they can do for the individual and what support services they can be signposted to.
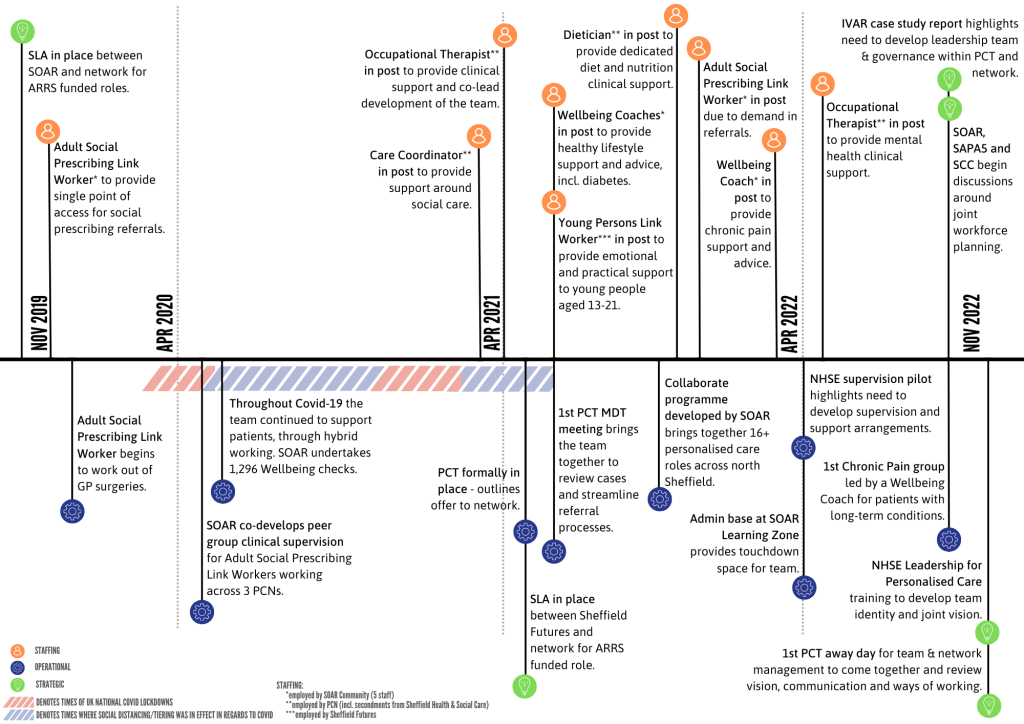
The timeline below demonstrates key stages of the SAPA 5 PCT development categorising and describing key staffing, operational and strategic milestones over the past two years.
Challenges
The case study categorised three current challenges of the SAPA 5 PCT Team and suggested ways to overcome these:
- Develop the PCT through better resourcing – adequate resourcing for governance, leadership and workforce development as the PCT evolves and grows. Whilst SOAR co-leads the development of the PCT, providing strategic and operational oversight of the PCT, including all-team training sessions & strategic design conversations. This is either unfunded (SOAR) or in addition to their clinical work (OT) who also oversees the team’s health and safety, and quality control. A fixed term Development Coordinator role is being considered, that would have the dedicated responsibility for helping to develop the PCT’s operational process and systems.
- Aligned policies and processes – individual roles are funded by and report to different organisations that can present challenges for the PCT colleagues understanding and adhering to a different set of policies and procedures. Adaptations to procedures are now being made to better meet client needs. E.g., when an organisation’s policy states their staff are not to make in-person visits to their clients in their homes, they have agreed these can be made when accompanied by an NHS colleague (whose policies support in-person visits).
- Greater mutual understanding of roles – there needs to be better and more consistent understanding of the role of the voluntary sector within the delivery of health and wellbeing services and support. This could be achieved through NHS professional and leadership development also being offered to voluntary sector colleagues taking on health leadership roles.
Achievements
The case study categorised three main achievements of the SAPA 5 PCT Team to date:
- Success in collaboration – demonstrated by the PCT team drawing on collective knowledge, experience, relationships, and networks from several organisations and industries.
- A smoother patient referral – a focus on understanding what the community needs and working as a team to work out ‘How can we provide a service?’ and taking a person-centred approach.
- A more holistic understanding of care – assisted health and voluntary sector colleagues to identify connections between social conditions and poor health. A few Wellbeing Coaches employed are coming from communities that they are working with which helps them to identify localised solutions and connect with patients from this commonality.
These achievements and similar have led to a very high retention of staff in the PCT employed through the Additional Role Reimbursement Scheme (ARRS) and showcases the great strength of working within a joint health/voluntary sector partnership.
Opportunities
The case study’s findings have begun the consideration for how we can develop a PCT leadership team that will work with the PCN Steering Group to showcase not only how the PCT works but also begin to help shape workforce development plans. This will provide a real opportunity to embed the operational and strategic partnership between SAPA5, SOAR and VCS partners over the next 5 years.
Reflections & testimonials
The following reflections are included in the case study and taken directly from SAPA 5 PCT Team.
“I think there is something really special about the partnership … the voluntary sector can do stuff that the NHS can’t, and all the sectors have something different to offer. I think it’s about figuring out how we work together, which is what we’re doing.”
NHS Worker (Page 5)
“It was like a breath of fresh air when we had that very first conversation, because you didn’t have to battle, you didn’t have to be defensive”
VCSE Worker (Page 6)
If you have any questions or would like to receive more information on the SAPA 5 PCT please contact [email protected] or [email protected]
